The New York Times – November 26, 2013
Two leading Shaare Zedek Medical Center doctors were featured in this article.
By RONI CARYN RABIN
November 26, 2013 289 Comments
KFAR SABA, Israel — Ever since she tested positive for a defective gene that causes breast cancer, Tamar Modiano has harbored a mother’s fear: that she had passed it on to her two daughters. Ms. Modiano had her breasts removed at 47 to prevent the disease and said that the day she found out her older daughter tested negative was one of the happiest of her life.
Now she wants her younger daughter, Hadas, 24, to be tested so she can start a family early if she is positive and then have a double mastectomy too. Ms. Modiano’s elder daughter, Suzi Gattegno, 29, disagrees.
“You’re keeping her from living her life,” Ms. Gattegno told her mother. “You want to marry her off early.”
“If she’s a carrier, she should marry early,” her mother countered.
Israel has one of the highest rates of breast cancer in the world. Mortality is very low, in part because of intense screening.
“She doesn’t even have a boyfriend,” the daughter said. “You need to stop pressuring her.”
“I want to protect her!” Ms. Modiano replied.
Such family debates are playing out across Israel these days. The country has one of the highest rates of breast cancer in the world, according to a World Health Organization report. And some leading scientists here are advocating what may be the first national screening campaign to test women for cancer-causing genetic mutations common among Jews — tests that are already forcing young women to make agonizing choices about what they want to know, when they want to know it and what to do with the information.
The so-called Jewish breast cancer genes have preoccupied women here for years, but after the actress Angelina Jolie revealed in May that she had undergone a double mastectomy because she had tested positive for such a mutation, coverage here exploded, with radio and TV talk shows featuring Israeli women grappling with similar decisions.
Jews of Ashkenazi, or central and eastern European, backgrounds, who make up about half the Jews in Israel and the vast majority of those in the United States, are much more likely to carry mutations that increase the risks for both breast and ovarian cancers, according to the National Cancer Institute.
A number of influential geneticists and cancer doctors from various medical centers here say that the Israeli Health Ministry should pay for free voluntary genetic testing of all Ashkenazi women over the age of 25. About a million women would be covered, at a cost of less than $100 per test. Jews of Iraqi descent, whose families also often carry a harmful mutation, might also be screened.
The goal of a proposed universal screening program would be to identify an estimated 30,000 Israeli women who have the mutations. So far, with sporadic testing, about 6,000 of them have been found, many only after a cancer diagnosis, said Dr. Ephrat Levy-Lahad, the coordinator of the Israel Genetics Consortium.
“That’s our target population,” said Dr. Oded Olsha, a breast surgeon at Shaare Zedek Medical Center in Jerusalem. “If we can find them, we can save their lives.”
Women who tested positive for mutations in the BRCA1 and BRCA2 genes, which suppress tumors, would be strongly encouraged to complete child bearing by their late 30s so they could have their ovaries removed by age 40. Risk-reducing mastectomies would also be offered.
The profoundly controversial idea of broad-based screening has already set off debate in Israel among advocates for women and those in the medical and scientific fields. Critics say it may lead to social stigma and a rash of unnecessary operations, and also burden some women with information they may not want or know how to use.
The choice is not a simple one. Removing the breasts and ovaries sharply reduces the risk of cancer, but mastectomies are disfiguring and women often experience scarring and numbness after breast reconstruction. Loss of the ovaries plunges women into menopause, potentially leading to hot flashes, a reduced sex drive and heightened risks of heart disease and bone loss.
But already demand for genetic testing is very high here — there are yearlong waiting lists — and national health insurance generally covers it as long as a woman is referred by her doctor or a genetic counselor.
While poor countries struggle to provide even basic cancer care to women, wealthier societies like Israel and the United States are increasingly using sophisticated technologies to identify those at greatest risk in an effort to thwart the disease before it gets started. Several American Jewish organizations have recently undertaken a campaign to raise awareness about the genetic susceptibility to breast and ovarian cancer among Ashkenazi Jews.
The cancer divide here in Israel is more ethnic than economic. Will only Ashkenazi Jews be routinely tested? Though they are much more likely to carry one of the common harmful mutations in the BRCA1 and BRCA2 genes, Israel is a melting pot of both Arab citizens and Jews from all over the world, and only half of the country’s six million Jews are of Ashkenazi ancestry.

Tali Shalev, 40, getting a CT scan at a hospital near Tel Aviv last month. Ms. Shalev, whose mother developed breast cancer at 50, tested positive for a genetic mutation. During a prophylactic double mastectomy, a cancerous lesion was found, and Ms. Shalev learned that the disease had spread to her bone.Rina Castelnuovo for The New York Times
Under the proposal being put forward by some Israeli geneticists, it is likely that Israeli Arab citizens and Jews of Sephardic ancestry — whose families originate in North Africa and the Middle East — would not routinely be included among those screened for BRCA mutations, a point of contention in a country where a social and ethnic rift already divides Sephardic and Ashkenazi Jews.
Families of Iraqi origin, like Ms. Modiano’s, may be covered because of their higher genetic risks. She always knew there was cancer in her father’s family. Three of his sisters died of breast cancer at young ages.
But she was tested for cancer-causing mutations only three years ago after finding out her relatives were being screened. The result stunned her.
“I thought about what it meant for me, and then I thought, ‘What about my daughters?’ ” Ms. Modiano said recently, shuddering slightly. “I was petrified. I still am.”
Within three months, Ms. Modiano had a risk-reducing double mastectomy and an operation to remove her ovaries. But the decisions facing her daughters, both in their 20s, were far more complicated. Neither was married, and each had a 50 percent chance of carrying the mutation.
Ms. Gattegno, who was in nursing school at the time, decided to be tested.
“I told my boyfriend that if I turned out to be a carrier, I would quit school for a while and we’d have kids right away,” she said. “And then I’d have a prophylactic mastectomy.”
Difficult Questions
At the Shaare Zedek Medical Center in Jerusalem, Dr. Levy-Lahad, who started one of the first genetic testing programs in Israel, is among the main champions of universal screening for Ashkenazi women. She has worked closely with the American scientist who identified the BRCA1 gene, Mary-Claire King.
“If you’re only testing women after they’ve been affected, you’ve lost the game,” Dr. Levy-Lahad said. “Genetic testing is about prevention.”
She pointed to the risks. One in 40 Ashkenazi women carry a harmful genetic mutation, compared to less than one in 100 women generally.
Women with these mutations are four to five times more likely to develop aggressive breast cancers, according to the National Cancer Institute. The disease often comes at an early age and in both breasts, said Dr. Gad Rennert, the director of Israel’s National Cancer Control Center.
The potential for preventing ovarian cancer, a rarer but more lethal disease, is even greater. The common harmful mutations found in Ashkenazis are implicated in about 30 percent of ovarian cancers in Israeli women — and 40 percent or more of cases in women under 60, Dr. Rennert said.
Practical and ethical questions abound. Should men — who are just as likely to pass the mutations to their children and who are themselves at increased risk for some cancers — also be tested? Will ultra-Orthodox Jews participate in screening, knowing a positive test could hurt their family’s chances of making a good marriage match?


Ms. Shalev, who has three children, kissed a prayer book and recited psalms after lighting the Sabbath candles at her home in Herzliya. In her bedroom, she rested with her mother, 4-year-old son and 12-year-old daughter.Rina Castelnuovo for The New York Times
Identifying people as carriers can change their perceptions of themselves and the way they envision their futures, said Dr. Gail P. Jarvik, the head of the division of medical genetics at University of Washington Medical Center in Seattle.
Even though the testing would be voluntary, women could feel pressured to participate, said Barbara A. Koenig, a professor of medical anthropology and bioethics at the University of California, San Francisco. “When you institute mass screening, you’re making a collective decision that this is a good thing.”
There are also lingering scientific questions. While much is known about the three common Ashkenazi BRCA1 and BRCA2 mutations, the risk they confer varies. Some families may have other genetic factors that modify their risk, which explains why some carriers never develop cancer while others die in their 20s.
Women identified as mutation carriers are showered with resources for early detection and prevention. These women’s risk for developing breast cancer ranges from 45 to 65 percent or higher, depending on family history, and their risk for ovarian cancer can be as high as 39 percent.
Routine mammography screening for most Israeli women starts at 50, but carriers are eligible for frequent clinical breast exams and expensive magnetic resonance imaging of the breast, all covered by national health insurance. They are also eligible for regular blood tests and vaginal ultrasounds to screen for ovarian cancer.
Cultural Obstacles
Many Israeli women who have the harmful mutations complain that male doctors display sexist attitudes about the importance of breasts and are loath to do mastectomies on healthy women.
Dr. Moshe Inbar, an outspoken oncologist in Tel Aviv who opposes preventive mastectomies, has said that a woman cannot have an orgasm after her breasts are removed, an assertion not supported by evidence.
“Would you like to live without your breasts?” Dr. Inbar, the director of the oncology division at Tel Aviv Sourasky Medical Center, asked. “I try to dissuade women from doing this. Surgery is not something that should be done on patient demand; it should be done when indicated.”
Women in Israel have a very high rate of breast cancer, but a very low rate of preventive mastectomies in those who carry the BRCA1 and BRCA2 mutations, which sharply increase the risk for developing breast cancer
Breast Cancer in Israel
Preventive mastectomy in women with BRCA1 and BRCA2 mutations
Breast cancer new cases per 100,000
While more than a third of American women carrying the harmful genetic mutations choose preventive mastectomies, only 4 percent of Israeli women do, according to a 2008 International Journal of Cancer study that compared risk-reducing procedures for samples of BRCA1 and BRCA2 mutation carriers in Canada, the United States, Israel and six European countries.
By contrast, well over half the carriers in all countries but Poland had their ovaries removed, a procedure that also reduces breast cancer risk.
But there are signs that attitudes are beginning to change here, as women take to the Internet to research their options, challenge the medical profession and shop for doctors.
Tamar Horesh, 35, a computer programmer from central Israel, has vivid memories of her mother’s painful death from ovarian cancer at 51.
When Ms. Horesh tested positive for a BRCA1 mutation, she said her husband supported her decision to surgically remove her ovaries and breasts. They had three young children to raise.
Finding a doctor to do it was another matter.
“The first doctor I went to said I was insane, and he said, ‘If you have brain cancer, are you going to chop off your head?’ ” said Ms. Horesh. “The second doctor said that he noticed I had a small chest, and he thought I just wanted an excuse to have my breasts enlarged.”
I remember it was like someone had slapped me in the face very hard. I could not believe it. ‘I am only 26 years old, this cannot be happening.’ But it all began.
A third doctor told her what many women hear, “Come back when you have cancer,” and “Nobody dies of breast cancer nowadays.”
In fact, some 900 Israeli women die of breast cancer each year, according to the Israel Cancer Association.
Ms. Horesh eventually got referrals from Bracha, a group founded to raise awareness by Lisa Cohen, who has a BRCA mutation.
Ms. Cohen’s mother died of cancer at 49, and then her sister, who had four young children, died at 36. “I felt like I was going to be next in line,” said Ms. Cohen, a divorced mother of three who was determined to stay alive for her children.
A Personal Decision
Hadas Modiano, a university student in Jerusalem, is waiting a couple of years before she seriously considers being tested as her mother insists. But her mother’s example has given her strength.
“I think I’m not as scared as I might have been because I saw what my mother went through,” she said. “It was hard, but she has managed and overcome.”

Ms. Shalev prayed for her children at the Tomb of Rachel on the outskirts of Bethlehem. According to Jewish tradition, prayers and tears are believed to have special powers at the tomb.Rina Castelnuovo for The New York Times
But for many women, the choices are harrowing. A Tel Aviv lawyer, 43, who asked that her name not be used to protect her privacy, was devastated when she found out at 26 that she had one of the bad mutations.
The lawyer, who was only 4 when her mother died of breast cancer, said she was among the first to line up for the genetic test when it became available in Israel in the 1990s.
“You may think you’re prepared for this information, but you aren’t,” she said. “My blood went cold when I found out.” Afterward, she said she realized, “The only solutions are so radical — amputating parts of your body.”
When she first met the man who became her husband, she told him that she could never marry or have children. He convinced her otherwise. She goes for frequent scans and checkups but postponed having a mastectomy so she could breast-feed their children.
She chose to become pregnant through in vitro fertilization so female embryos that did not carry harmful mutations could be selected in the lab.
“Finally, there was something positive to do with the information,” she said.
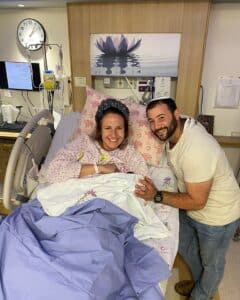
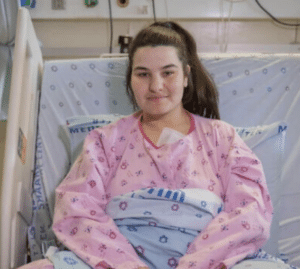
Preventive surgeries are not always successful. Tali Shalev had what was supposed to be a preventive double mastectomy, but pathologists found a cancerous lesion in the removed breast tissue. “I’m an example of someone who did everything possible,” said Ms. Shalev, 40, who has three children.

Removing the breasts sharply reduces the risk of cancer in women with genetic mutations. Still, mastectomies are disfiguring and after breast reconstruction, women often experience numbness. Above, after a double mastectomy and reconstruction.Rina Castelnuovo for The New York Times
The dilemmas of genetic testing are compounded in the ultra-Orthodox community, where the emphasis on modesty often dampens open discussion.
Still, Tziporah, 38, a Canadian-born Orthodox mother of seven who now lives in Israel, talks openly about her experience because she wants to reach other religious women. Tziporah, who goes by her nickname, Tzippy, asked that her last name not be used to protect the privacy of her extended family members, who also may carry the gene. Her mother died of breast cancer at 42, when she was 5, and when Tzippy was pregnant with her last child a few years ago, she tested positive for a BRCA1 mutation.
She sought advice from several rabbis about whether she should go forward with risk-reducing surgeries. They reassured her that preserving life is one of the supreme values of Judaism.
So three years ago, after her youngest child was born, she had her breasts and ovaries removed. The operations were grueling, but she said she wanted to make sure her children would not suffer the same loss she had. And she said she felt she had a mission to encourage other women to be tested.
“You know why God did this to me?” she said. “Because I’ve got a really big mouth.”
So she is spreading the word within the Orthodox community that genetic screening can save lives.
“Women don’t have to be dying on their kids,” she said.